The modern doctor office has evolved far beyond a simple waiting room and examination space. Today's primary care facilities must balance patient expectations, operational efficiency, advanced technology integration, and comprehensive care coordination. Whether you're managing an established practice or planning a new facility, understanding the core principles that make a doctor office successful is essential for delivering exceptional patient experiences while maintaining profitability and staff satisfaction.
Essential Management Practices for Medical Offices
Running an efficient doctor office requires systematic approaches to daily operations. The foundation starts with clear leadership and well-defined organizational structures that empower every team member to contribute to patient care excellence.
Streamlining Administrative Workflows
Modern doctor office operations depend heavily on reducing administrative burden. Insurance verification before appointments prevents billing surprises and improves patient satisfaction. Pre-visit verification allows staff to identify coverage issues, confirm copays, and address potential payment concerns before patients arrive.
Key administrative efficiencies include:
- Automated appointment reminders via text, email, and phone
- Digital intake forms accessible from patient portals
- Real-time eligibility verification systems
- Centralized scheduling across multiple providers
When administrative staff can focus on these effective management practices for doctors’ offices, clinicians gain more time with patients. This division of labor ensures medical professionals concentrate on clinical care while support teams handle operational tasks.

The integration of ancillary services within a single doctor office creates additional coordination requirements. Labs, imaging, physical therapy, and specialty consultations must flow seamlessly. Digital systems that connect these services reduce duplicate data entry and minimize errors.
Technology Integration and Staff Training
Investing in the right technology transforms doctor office efficiency, but only when paired with comprehensive staff training. Electronic health records (EHR), practice management systems, and patient communication platforms require ongoing education to maximize their value.
According to best practices for managing a physician’s office, staying current with technology prevents operational bottlenecks. Regular training sessions ensure staff members use systems to their full potential rather than developing workarounds that decrease efficiency.
| Technology Area | Primary Benefit | Implementation Priority |
|---|---|---|
| Patient Portal | Self-service access to records, appointments | High |
| EHR Integration | Reduced documentation time, better coordination | Critical |
| Telehealth Platform | Expanded access, convenience | Medium |
| Automated Billing | Faster reimbursement, fewer errors | High |
| Inventory Management | Optimal supply levels, cost control | Medium |
Designing Patient-Centered Spaces
The physical environment of a doctor office significantly impacts patient comfort, anxiety levels, and overall satisfaction. Thoughtful design considers every touchpoint in the patient journey, from parking lot to checkout.
Creating Welcoming Entry Points
First impressions matter tremendously in healthcare settings. The entrance to a doctor office should communicate professionalism, cleanliness, and warmth simultaneously. Clear signage reduces confusion and anxiety for new patients, while accessible design ensures everyone can enter comfortably.
Research on medical office design for patient comfort shows that natural lighting, comfortable seating, and calming colors reduce patient stress. These elements are particularly important for primary care practices serving all age groups, where pediatric patients and elderly visitors may have different comfort needs.
Modern waiting areas function as transitional spaces rather than holding pens. Strategic placement of check-in desks allows privacy during registration. Separate areas for well visits and sick appointments prevent exposure concerns, particularly relevant for practices offering same-day appointments where acute illnesses are common.
Optimizing Clinical Workflow Through Design
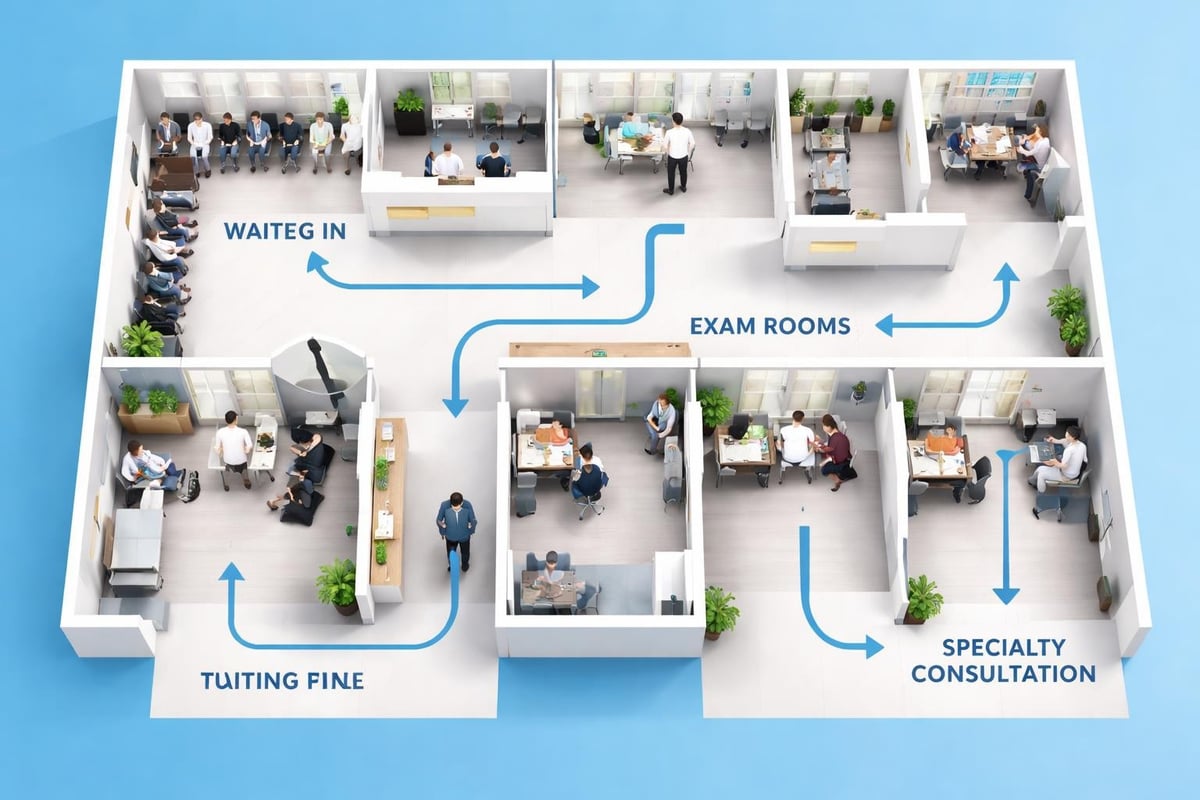
Behind-the-scenes layout dramatically affects doctor office efficiency. The arrangement of examination rooms, nursing stations, and support spaces determines how smoothly staff can move through daily tasks.
Critical workflow considerations:
- Centralized nursing stations equidistant from exam rooms
- Strategic placement of supplies to minimize steps
- Private consultation spaces separate from exam areas
- Efficient paths between clinical and administrative zones
The current trends in medical office design emphasize flexibility and future-proofing. As healthcare delivery models evolve, doctor office spaces must adapt to new technologies, team-based care models, and hybrid in-person/virtual service delivery.
When primary care practices incorporate multiple specialties and ancillary services, dedicated zones prevent operational conflicts. Lab draw stations, imaging suites, and procedure rooms require specific infrastructure while maintaining easy access from the main clinical flow.
Enhancing Patient Experience Through Operational Excellence
Patient satisfaction extends beyond clinical outcomes to encompass every interaction with the doctor office. From initial phone contact through follow-up care, each touchpoint contributes to overall perception.
Communication Standards and Accessibility
Clear, consistent communication defines exceptional patient experiences. Staff training should emphasize empathetic listening, plain-language explanations, and proactive information sharing. When patients understand their care plans, they're more likely to follow recommendations and achieve better health outcomes.
The ability to offer same-day appointments addresses a major patient frustration with traditional doctor office scheduling. Reserving capacity for urgent needs demonstrates responsiveness while requiring sophisticated scheduling systems to balance planned and acute care.
According to patient experience best practices, safety and transparency build trust. Patients want to know what to expect during visits, how long procedures take, and what happens after they leave the doctor office. Digital communication tools enable pre-visit education and post-visit follow-up without burdening office phone lines.
Coordinating Comprehensive Care Services
Primary care practices serving as medical homes must coordinate various services seamlessly. When a doctor office offers in-house labs, imaging, and specialty consultations, internal referral processes need careful management.
Coordination best practices include:
- Standardized referral templates with complete clinical information
- Direct scheduling assistance for specialty appointments
- Shared documentation accessible across service lines
- Follow-up tracking to ensure patients complete recommended care
- Care team huddles to discuss complex cases
The integration of multiple services under one roof provides convenience but increases operational complexity. Staff members need cross-training to understand how different departments function and where to direct patients. For healthcare practices looking to expand their patient base, partnering with specialists like RevSpark Media can help optimize lead generation and patient onboarding systems while maintaining focus on care delivery.
Staff Development and Team Culture
The success of any doctor office ultimately depends on its people. Hiring qualified staff represents just the first step; ongoing development and positive workplace culture determine long-term performance.
Building High-Performing Medical Teams
Top management practices for successful medical offices emphasize leadership development at all levels. While physicians provide clinical direction, practice managers, nursing supervisors, and administrative leads shape daily operations.
Regular team meetings create opportunities for problem-solving, celebrating successes, and addressing concerns before they escalate. When staff members understand how their roles contribute to patient outcomes, engagement increases dramatically.
| Position | Key Competencies | Development Focus |
|---|---|---|
| Front Desk | Customer service, multitasking | Communication skills, software training |
| Medical Assistants | Clinical skills, documentation | Specialty procedures, EHR optimization |
| Nursing Staff | Patient assessment, care coordination | Advanced certifications, leadership |
| Administrative | Billing, compliance, operations | Regulatory updates, process improvement |
Cross-training creates operational resilience. When multiple team members can perform critical functions, the doctor office maintains service levels during absences. This flexibility is particularly valuable for smaller practices where each person plays multiple roles.
Maintaining Work-Life Balance and Reducing Burnout
Healthcare professionals face significant stress, and doctor office management must prioritize staff wellbeing. Reasonable schedules, adequate break times, and supportive policies prevent burnout that leads to turnover and diminished patient care.
Creating systems that allow clinicians to focus on patients rather than paperwork improves job satisfaction. When administrative tasks are handled efficiently by support staff, physicians can practice at the top of their licenses. This division of responsibility benefits everyone, from staff members to the patients they serve.

Implementing Quality Improvement Initiatives
Continuous improvement distinguishes excellent doctor offices from merely adequate ones. Systematic approaches to measuring performance, identifying gaps, and implementing changes drive better outcomes over time.
Measuring Patient Satisfaction and Clinical Outcomes
What gets measured gets managed. Regular patient satisfaction surveys provide actionable feedback about doctor office performance. Beyond general satisfaction scores, specific questions about wait times, staff courtesy, facility cleanliness, and communication clarity reveal improvement opportunities.
Clinical outcome tracking ensures the doctor office delivers effective care. For primary care practices, metrics might include chronic disease management indicators, preventive care completion rates, and hospital readmission statistics.
Essential performance metrics:
- Average wait time from arrival to provider
- Patient satisfaction scores across service dimensions
- Appointment availability for urgent and routine needs
- No-show and cancellation rates
- Clinical quality measures for preventive and chronic care
Data collection means nothing without action. Monthly reviews of performance dashboards should trigger specific improvement initiatives. When trends emerge, whether positive or negative, understanding root causes enables targeted interventions.
Creating Feedback Loops and Accountability
Staff members closest to operations often identify improvement opportunities that management overlooks. Creating formal channels for suggestions and concerns demonstrates respect for frontline expertise while generating valuable ideas.
Implementing changes requires clear ownership and accountability. When the doctor office decides to modify a process, designating a specific person to lead the initiative increases success rates. Regular check-ins assess progress and address obstacles.
The principles outlined in resources about improving office design to enhance patient experience apply to operational improvements as well. Small, incremental changes often yield significant results without requiring major investments or disruptions.
Financial Management and Sustainability
Even the most patient-centered doctor office must maintain financial health to continue serving the community. Sound financial practices ensure long-term viability while supporting investment in staff, technology, and facilities.
Revenue Cycle Optimization
Efficient billing and collections directly impact doctor office profitability. Clean claims submission, prompt follow-up on denials, and patient payment collection at time of service all contribute to healthy cash flow.
Prior authorization requirements create administrative burden but cannot be ignored. Dedicated staff members who understand insurance requirements and maintain positive relationships with payers expedite approvals and reduce delays.
For practices offering ancillary services, understanding the profitability of each service line guides resource allocation. Some services may operate at lower margins but provide patient convenience that supports overall practice growth.
Strategic Planning and Growth Management
As communities evolve, doctor offices must adapt to changing demographics, competitive pressures, and healthcare delivery trends. Strategic planning processes assess market opportunities, capacity constraints, and expansion possibilities.
Same-day appointment availability requires careful capacity management. Balancing scheduled visits with reserved slots for acute needs prevents overwhelming providers while meeting patient expectations for accessibility. Resources from Dominion health demonstrate how integrated primary care practices successfully manage this balance.
Growth opportunities might include expanding hours, adding providers, incorporating new services, or opening additional locations. Each option requires analysis of market demand, financial feasibility, and operational readiness. Successful expansion maintains the quality standards and patient relationships that define the existing doctor office while extending reach.
Creating an exceptional doctor office requires attention to management practices, physical design, patient experience, staff development, quality improvement, and financial sustainability. These elements work together to deliver accessible, high-quality primary care that meets diverse patient needs. At Dominion health, we've built our practice around these principles, offering comprehensive primary care for all ages with in-house ancillary services, subspecialty support, and same-day appointment availability. Whether you need routine preventive care or urgent medical attention, our integrated approach ensures you receive coordinated, convenient care when you need it most.
