With healthcare changing at an unprecedented pace, selecting the right primary care provider is more important than ever in 2026. Many patients, medical students, and professionals are asking how to navigate the choice between internal medicine family practice.
This article breaks down the main differences between these two specialties. You will learn about their training, patient demographics, scope of practice, chronic disease management, and what the future holds for each path.
By the end, you will have the clarity needed to make informed decisions for yourself, your loved ones, or your career.
Definitions and Core Focus of Internal Medicine vs Family Practice
Understanding the distinction between internal medicine family practice is crucial for patients and healthcare professionals. Both fields are pillars of primary care, yet their approaches, patient populations, and philosophies differ in meaningful ways. Let us explore these differences to help clarify which specialty best aligns with specific healthcare needs.

What is Internal Medicine?
Internal medicine family practice involves a specialized focus on adult patients, beginning at age 18 and continuing through senior years. Internists are trained to prevent, diagnose, and manage diseases that commonly affect adults, often handling complex or multiple chronic conditions.
Internists frequently work with subspecialties such as cardiology, gastroenterology, and endocrinology, providing in-depth expertise. For example, an internist may oversee a patient with diabetes, heart disease, and hypertension simultaneously, ensuring coordinated care. According to the AAMC, 70 percent of internists practice in outpatient settings, emphasizing their role as "doctors for adults." This depth of training shapes the internal medicine family practice approach, making it ideal for adults with intricate health needs.
What is Family Practice?
Family practice within the internal medicine family practice discussion takes a broad approach, caring for individuals of all ages, from newborns to seniors. Family physicians are generalists, trained to handle a wide range of conditions, preventive care, and both acute and chronic illnesses.
Their patient population spans entire families, often providing care to multiple generations. It is common for a family physician to treat a child’s asthma, a parent’s hypertension, and a grandparent’s arthritis. Notably, the AAFP reports that 80 percent of family physicians provide pediatric care. Family doctors are seen as “whole-family care providers,” reflecting the comprehensive nature of internal medicine family practice for every life stage.
Key Philosophical Differences
The core philosophy of internal medicine family practice centers on either depth or breadth. Internal medicine emphasizes specialization in adult health, focusing on complex diseases and continuity for adults. Family practice, on the other hand, prioritizes continuity across all ages, life transitions, and preventive care.
For instance, family physicians often guide patients through childhood, adolescence, pregnancy, and aging, while internists focus on managing adult diseases. Leading organizations like the ACP and AAFP have highlighted that these philosophical differences impact patient satisfaction and long-term relationships. For a comprehensive comparison of these two specialties, you can refer to Internal Medicine vs. Family Medicine: What’s the Difference?. Choosing between internal medicine family practice options can significantly affect the patient experience.
Overlapping Areas and Collaboration
Despite their differences, internal medicine family practice overlap in several key areas. Both serve as primary care providers for adults, manage chronic diseases, and advocate for preventive care. Collaborative efforts in multi-specialty clinics and referral networks are common, especially in managing complex cases like diabetes.
For example, a family doctor may consult with an internist for an adult patient with multiple health issues, ensuring comprehensive treatment. According to the AMA, 60 percent of family physicians collaborate with internists for complex adult cases. This integrated approach in internal medicine family practice benefits patients by delivering coordinated and holistic care.
Education, Training, and Certification Pathways
Choosing between internal medicine family practice starts with understanding the education and training each path requires. While both specialties begin with a medical degree (MD or DO), their journeys diverge after graduation, shaping the skills and scope of future physicians.
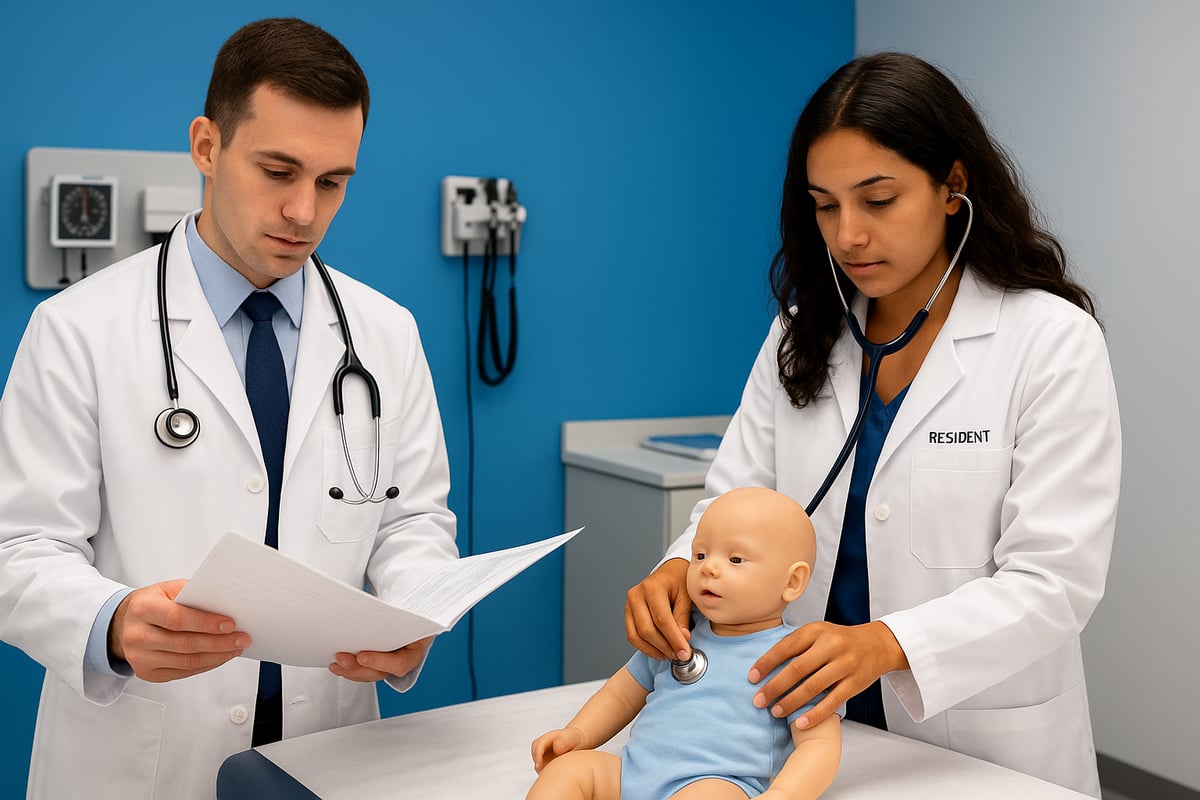
Medical School and Residency Requirements
Both internal medicine family practice physicians must complete four years of medical school. Afterward, they enter specialized residency programs lasting three years, but the content and focus differ significantly.
Here is a comparison table summarizing the key differences:
| Training Step | Internal Medicine | Family Practice |
|---|---|---|
| Medical School | MD/DO (4 years) | MD/DO (4 years) |
| Residency | 3 years (adults only) | 3 years (all ages, including OB/GYN) |
| Pediatric Training | Limited | Extensive |
| OB/GYN Training | None | Required |
| Inpatient Experience | Significant | Moderate |
Internal medicine residents train exclusively with adults, focusing on complex cases in both outpatient and hospital settings. Family practice residents rotate through pediatrics, obstetrics, geriatrics, and behavioral health, gaining experience with patients at every life stage.
Board certification is required for both, but the process varies. For those interested in the family medicine pathway, review the Family Medicine Residency Training Requirements for a detailed breakdown of the process.
Understanding the demands and structure of each residency helps medical students choose the right internal medicine family practice path for their goals.
Subspecialization and Fellowships
After residency, internal medicine family practice physicians may pursue further specialization. Internal medicine offers a wide range of fellowships, including:
- Cardiology
- Gastroenterology
- Oncology
- Endocrinology
- Infectious Disease
Family practice has fewer fellowship options, but popular choices include:
- Sports Medicine
- Geriatrics
- Adolescent Medicine
The ability to subspecialize can significantly impact a physician's career. For example, an internal medicine doctor may become a cardiologist, while a family practice doctor might focus on sports medicine. This flexibility is a key consideration when comparing internal medicine family practice options.
Continuing Medical Education (CME) and Recertification
Both internal medicine family practice doctors must engage in lifelong learning. Continuing Medical Education (CME) is a requirement for maintaining board certification.
Key points for both specialties:
- Regular CME credits (often annually)
- Recertification exams every 7–10 years (e.g.,
board exam: every 10 years) - Staying updated on guidelines and best practices
According to recent data, 95% of internists maintain their board certification, showing a strong commitment to ongoing education. The internal medicine family practice commitment to CME ensures high standards of care for patients.
Training Focus: Depth vs. Breadth
The core distinction between internal medicine family practice training lies in scope. Internal medicine focuses deeply on adult diseases, with extensive exposure to hospital medicine and complex cases. Residents gain expertise in managing multiple chronic illnesses, rare conditions, and acute adult emergencies.
Family practice emphasizes breadth, preparing doctors to care for newborns, children, adults, and seniors. Their training covers behavioral health, preventive care, minor procedures, and pediatric immunizations. This broad foundation allows family physicians to address diverse medical needs in a single practice.
In daily practice, this means internal medicine family practice doctors bring different strengths to the table. Family doctors excel in continuity and comprehensive care, while internists provide in-depth expertise for adult patients with complex needs.
Patient Demographics and Scope of Practice
Understanding the patient demographics and scope of practice is essential when comparing internal medicine family practice. These factors influence the care each specialty provides, shaping the experiences of both patients and physicians.

Age Groups and Patient Types
Internal medicine family practice caters to distinct patient populations. Internists primarily treat adults aged 18 and older, focusing on those with complex or chronic illnesses. In contrast, family physicians provide care for individuals across the entire lifespan, from newborns to seniors.
For example, a family doctor might care for a child with asthma, a parent with diabetes, and a grandparent with hypertension, often within the same family. This broad approach allows for continuity and convenience, especially for families seeking one trusted provider. According to the American Academy of Family Physicians, 90% of family physicians see pediatric patients as part of their practice in 2025.
This wide-ranging patient base is a defining feature of internal medicine family practice, shaping the services and relationships developed over time.
Types of Conditions Treated
The spectrum of conditions managed by internal medicine family practice reflects each specialty’s training and patient focus. Internists are experts in diagnosing and treating complex adult diseases such as diabetes, heart disease, and cancer. Their in-depth knowledge supports patients with multiple or difficult-to-manage health issues.
Family physicians, meanwhile, address a broader range of concerns. They manage acute infections, minor injuries, preventive screenings, and chronic diseases for patients of all ages. For instance, a family doctor may treat a child’s ear infection in one appointment and address an adult’s hypertension in the next.
For more detailed insights into how both specialties provide primary care for adults, consider the specific services offered in each setting.
Preventive Care and Wellness
Preventive care is a cornerstone of internal medicine family practice, but each specialty takes a unique approach. Family physicians emphasize immunizations, well-child visits, reproductive health, and lifestyle counseling for patients at every life stage. This proactive care aims to prevent illness before it starts.
Internists focus preventive efforts on adult patients, conducting screenings such as colonoscopies, cholesterol checks, and cancer risk assessments. While both specialties encourage wellness, family doctors often provide prenatal care and pediatric immunizations, reflecting their broader patient base.
According to recent data, 85% of family physicians offer preventive women’s health services, underscoring their commitment to comprehensive wellness.
Chronic Disease Management
Managing chronic disease is central to internal medicine family practice. Internists often care for adults with complex, multi-system illnesses like advanced heart failure, chronic kidney disease, or uncontrolled diabetes. Their specialized training prepares them to handle intricate cases and coordinate with subspecialists.
Family physicians also manage chronic conditions, but across all age groups. A family doctor may oversee a child’s asthma, an adolescent’s depression, and an adult’s diabetes within the same practice. This continuity supports early intervention and coordinated care for families managing multiple health challenges.
Both specialties strive to improve quality of life for patients living with chronic disease, adapting their approach to the needs of their specific patient populations.
Inpatient vs. Outpatient Care
The settings where internal medicine family practice delivers care differ significantly. Internists are more likely to provide hospital-based (inpatient) care, especially for adults with serious or acute conditions. This includes managing patients during hospital stays and coordinating discharge planning.
Family physicians typically work in outpatient clinics, community health centers, or private practices. However, in rural areas, family doctors may also provide inpatient care, ensuring access for underserved populations. Data from Medscape in 2025 indicates that 60% of internists provide inpatient care, compared to just 20% of family physicians.
These differences affect continuity of care and patient experiences, highlighting the importance of choosing the right primary care provider for individual needs.
Practice Settings and Daily Work Life in 2026
The daily experience of internal medicine family practice professionals in 2026 is shaped by their unique work environments, patient populations, and evolving technology. Understanding these differences can help both patients and practitioners make informed choices about care and career paths.
Typical Practice Environments
Internal medicine family practice physicians work across a spectrum of settings. Internists are commonly found in hospitals, multispecialty clinics, and private practices, especially in urban areas. In contrast, family physicians often serve in community clinics, private offices, and rural health centers, where they may be the primary source of care for entire communities.
For example, a family doctor in a small town might manage everything from newborn checkups to elderly care, while an internist in a city hospital focuses on adult patients with complex conditions. The internal medicine family practice landscape in 2026 reflects ongoing efforts to offer accessible care in diverse locations, ensuring both specialties remain vital to the healthcare system.
Patient Volume and Visit Types
Patient volume and visit types differ between internal medicine family practice roles. Family physicians typically see a higher number of patients each day, averaging 20 to 25 visits, focusing on preventive care, acute illnesses, and routine checkups. Internists, on the other hand, manage 15 to 20 patients daily, often spending more time with each due to the complexity of adult diseases.
This distinction means family doctors address a broad array of conditions quickly, while internists dedicate longer visits to in-depth management of chronic issues. The internal medicine family practice workflow is tailored to meet the unique needs of their respective patient populations, balancing efficiency with comprehensive care.
Use of Technology and Telemedicine
In 2026, technology plays a central role in internal medicine family practice. Both specialties have embraced telemedicine for follow-ups, chronic disease management, and even routine wellness visits. Family physicians frequently use virtual platforms for well-child appointments and mental health consults, making care more accessible to busy families.
Internists leverage telehealth for monitoring chronic conditions, utilizing tools like remote blood pressure cuffs and diabetes trackers. The integration of digital health solutions has transformed the internal medicine family practice environment, allowing for better communication, timely interventions, and enhanced patient engagement.
Work-Life Balance and Burnout
Work-life balance is a critical consideration in internal medicine family practice. Family physicians often enjoy greater flexibility, with regular office hours and fewer overnight calls, which can contribute to better overall well-being. Internists, particularly those involved in hospital care, may face higher rates of burnout due to demanding schedules and complex patient cases.
Recent data indicate that 48% of internists report symptoms of burnout, compared to 38% of family physicians. The internal medicine family practice profession continues to seek innovative ways to support provider wellness, including team-based care models and improved scheduling strategies to reduce stress and enhance job satisfaction.
Compensation and Job Satisfaction
Compensation and satisfaction levels vary within internal medicine family practice. On average, internists earn slightly more, with annual incomes around $270,000 compared to $250,000 for family physicians. However, family doctors often report higher satisfaction with patient relationships and continuity of care.
Factors influencing compensation include location, subspecialty, and practice setting. Urban internists may see higher earnings, while rural family physicians value the deep connections they form with patients. For a closer look at how practice styles and charges differ between these specialties, see this study comparing family physicians and general internists. Ultimately, internal medicine family practice professionals find fulfillment in different aspects of their roles, reflecting the diverse opportunities within primary care.
Choosing Between Internal Medicine and Family Practice: Patient and Physician Perspectives
Selecting between internal medicine family practice providers in 2026 involves critical choices for patients and physicians alike. Both specialties play vital roles in primary care, yet each offers distinct benefits based on individual needs and career goals. Understanding these differences can empower patients to find the right provider and guide medical professionals in shaping their careers.
Patient Decision Factors
When deciding between internal medicine family practice, patients often consider age, health needs, and family structure. For example, young families may prefer one doctor for all members, while adults with multiple chronic conditions might seek an internist’s expertise.
A recent survey revealed 60% of patients choose family doctors for convenience and continuity. Patients also value board certification, accessibility, and communication style. For those interested in comprehensive family care, the Family Practice Group Overview provides more details on available services and what to expect from family physicians.
Physician Career Considerations
Physicians weighing internal medicine family practice careers focus on their interests and future goals. Those passionate about caring for specific age groups or managing complex adult conditions often gravitate toward internal medicine. In contrast, doctors who enjoy working with all ages and building long-term relationships may prefer family practice.
Subspecialization is another consideration. Internists have broader options for fellowships, while family physicians typically remain generalists. For more insights into the daily work and expectations in internal medicine, visit Internal Medicine Doctor Insights.
Accessibility and Availability in 2026
Access to internal medicine family practice varies by location. Family physicians are more prevalent in rural and underserved areas, providing 65% of rural primary care. Internists are typically found in urban and suburban centers, where patient populations may require specialized adult care.
Patients in rural regions benefit from the broad skills of family doctors, while those in cities may have greater access to internal medicine expertise. This distribution ensures that communities receive appropriate primary care, regardless of geography.
Impact on Healthcare Outcomes
Both internal medicine family practice specialties contribute to improved healthcare outcomes. Family medicine is associated with lower healthcare costs, enhanced preventive care, and better community health. Internists excel in managing complex adult cases, leading to positive results for patients with multiple health issues.
Communities with a higher concentration of family physicians often experience reduced hospitalization rates. Meanwhile, internists provide specialized management for adults with chronic or critical conditions, supporting better individual outcomes.
How to Find the Right Primary Care Provider in San Antonio
Finding the right internal medicine family practice provider involves reviewing credentials, patient feedback, and service availability. Many patients prefer clinics offering both specialties, as this supports seamless care for all ages.
Dominion Health in San Antonio exemplifies this integrated approach, providing comprehensive care, same-day appointments, and subspecialty support. Choosing a provider focused on patient relationships and accessibility ensures the best experience for local residents.
Future Trends: Internal Medicine and Family Practice in 2026 and Beyond
As healthcare moves forward, internal medicine family practice is evolving rapidly. The next few years will bring significant changes in how primary care is delivered, who provides it, and the tools available to both patients and physicians. Understanding these trends is essential for anyone navigating the healthcare landscape in 2026.
Evolving Roles in Healthcare Teams
The lines between internal medicine family practice and other primary care roles are blurring. In 2026, healthcare teams are more collaborative than ever. Family doctors are often at the center of patient-centered medical homes, coordinating care with nurse practitioners and physician assistants.
Internists are increasingly specializing in hospital medicine, managing complex adult cases alongside multidisciplinary teams. Both specialties are essential in integrated clinics, ensuring continuity and comprehensive care. These evolving roles allow for better patient outcomes and more efficient use of resources.
Advances in Preventive Care and Technology
Technology is transforming internal medicine family practice, making preventive care smarter and more accessible. Remote monitoring tools and wearable devices enable real-time tracking of chronic conditions like diabetes and hypertension. Artificial intelligence helps physicians identify risks earlier and personalize treatment plans.
Family practice clinics are using digital health platforms to promote wellness, while internists leverage telemonitoring for advanced disease management. For those interested in subspecialty pathways, you can learn more about the latest requirements at Internal Medicine Subspecialty Policies. These advances improve patient engagement and drive better health outcomes.
Policy Changes and Healthcare Access
Policy shifts are shaping the future of internal medicine family practice. Governments and insurers are expanding value-based care models, rewarding clinics for preventive services and positive health outcomes. As a result, more patients can access screenings and essential care.
Recent data shows a 20 percent increase in preventive screenings since 2022, reflecting successful policy efforts. Expanded insurance coverage and government investment in primary care are helping reduce barriers, especially for underserved populations. These changes are essential for building a healthier society.
Addressing Physician Shortages
The demand for internal medicine family practice physicians continues to grow. Primary care deserts, especially in rural areas, highlight the need for more providers. National initiatives are underway to attract medical students to both specialties, with a projected 10 percent shortage of primary care physicians by 2030.
Efforts include loan repayment programs, flexible training pathways, and incentives for practicing in underserved communities. Addressing these shortages is crucial for maintaining access and quality in primary care across the country.
Patient-Centered Innovations
Patient needs are driving innovation in internal medicine family practice. Clinics are adopting personalized medicine, using genetic and lifestyle data to tailor care. Culturally competent services and expanded telehealth options address diverse populations and busy schedules.
Family practices are enhancing mental health support and addressing social determinants of health. Internal medicine is leading advances in precision medicine for chronic conditions. For a deeper look at the breadth of care in family medicine, see General Family Medicine Explained. Integrated behavioral health and coordinated care models ensure that patients receive comprehensive, convenient services.
As you consider the differences between internal medicine and family practice in 2026, remember that choosing the right primary care provider truly shapes your health journey. Whether you need care for yourself, your children, or an aging parent, having access to same day appointments, in house services, and sub specialty support means you receive comprehensive, timely care when it matters most. If you're ready to take the next step toward personalized, patient centered healthcare, you can easily Book Appointment and connect with a team dedicated to supporting your well being at every stage of life.
